Finally....Medicare Reference Pricing embedded in my Population Health Analytics application!
 The more time I spent in the field this past spring, the more I heard from both existing and potential clients about the need to analyze plan allowed amounts against Medicare pricing equivalencies. It's no secret that employers, brokers, consultants, TPA's and health plans are all considering various reference-based or Medicare-based pricing strategies in their plan designs. Whether considering a total PPO replacement, a narrow network strategy complemented with Medicare pricing wrapped around it, replacing your traditional out-of-network strategy (supplemental PPO aggregators and fee negotiation firms) with a Medicare pricing approach, or eliminating certain high cost providers from the network, all of these strategies require you to answer this simple question - "What am I paying as compared to a factor of Medicare reimbursement?".
The more time I spent in the field this past spring, the more I heard from both existing and potential clients about the need to analyze plan allowed amounts against Medicare pricing equivalencies. It's no secret that employers, brokers, consultants, TPA's and health plans are all considering various reference-based or Medicare-based pricing strategies in their plan designs. Whether considering a total PPO replacement, a narrow network strategy complemented with Medicare pricing wrapped around it, replacing your traditional out-of-network strategy (supplemental PPO aggregators and fee negotiation firms) with a Medicare pricing approach, or eliminating certain high cost providers from the network, all of these strategies require you to answer this simple question - "What am I paying as compared to a factor of Medicare reimbursement?".
Today, answering this question takes a lot of time and manual effort, and the comparison output is often inaccurate and unreliable, as regional pricing, place of service, gap-filling when no Medicare price exists, and other factors need to be taken into account for an accurate comparison. Payers are typically requested to build a historical claims extract, then send it via a secure method to a Medicare pricing vendor. That vendor has to map the data, ensure all required fields are present, and then schedule a job to run the data against Medicare pricing. The vendor then has to review the output and prepare summary reports, which may or may not include various increments of Medicare, and present the findings back to the payer. As you can imagine, this process typically takes weeks, and that's assuming the data is clean the first time around and the request is handled timely by all parties.
One of the advantages we have here at Deerwalk is the flexibility of our NoSQL Big Data technology stack. It allows for agile software development and continuous innovation, resulting in frequent sprint releases that update the applications with new features and functionality. We take that innovation seriously. We have a standing monthly meeting to discuss new ideas and features that have been brought to our attention by our clients, and rank order those concepts for future development. This allows us to steer development in the direction of what's most important to our clients and the market in general. As a matter of fact, we dedicate over 20,000 hours a month and over 120 employees to R&D and product development alone. Now that's a commitment!

One such idea, Medicare Reference Pricing, was born out of one of those brainstorming sessions a few months ago. I brought feedback from my time in the field to the product team, and just a few short months later - Voilà! - Agile Development in action! We are now excited to announce that Deerwalk's Plan Analytics is the first Population Health Management platform that has simplified the arduous process described above by fully integrating and automating accurate Medicare benchmark pricing information directly into the Plan Analytics application.
Here's How It Works:
Upon implementation, Deerwalk will run initial claims history against Medicare pricing information and refresh new claims data with Medicare pricing equivalencies as the data comes in (usually monthly). This allows clients to run on-the-fly reports and ad-hoc "what if" scenarios at the line level, claim level, group level, provider level, network level (in vs out) and service type, by comparing allowed amounts to five increments of Medicare reimbursement (100%, 125%, 150%, 175%, and 200%). This allows our clients to save a lot of time doing analyses for each group or line of business that may be considering a Medicare pricing strategy.
Here Are The Benefits:
- Real time analyses of allowed amounts against Medicare benchmarks, at the line level
- Run In and Out-of-Network scenarios against Medicare at different levels
- Determine providers and service categories with highest allowed amounts compared to Medicare at different levels
- Understand potential savings at each level of Medicare-based reimbursement — 100%, 125%, 150%, and 200%
- Evaluate network exclusions, narrow network and steerage targets, and plan design changes
- Ask "what if" scenarios for Medicare pricing Identify gap filling opportunities for services that do not have a Medicare-specific rate
- Inclusion of 16 Medicare fee schedules by provider type
Here's a screen shot of the application in action (keep in mind this is demo data, so some of the factors may look a little funky):
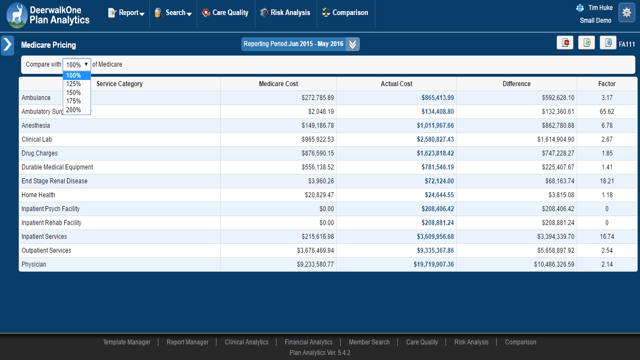
We are really excited about this new feature. The reaction from the market has been tremendous. To learn more about Deerwalk's Population Health Analytics Solutions, including Medicare Reference Pricing, please visit us at Deerwalk, or if you would like to schedule a demo, click below.


